India is preparing to take a decisive leap in women’s healthcare with a nationwide free HPV vaccination drive aimed at eliminating cervical cancer. Beginning March 2026, the Union government will roll out a 90-day campaign to administer a single dose of Gardasil-4 to 14-year-old girls across the country. The move signals not just a policy shift, but a public health milestone—one aligned with global scientific consensus and the World Health Organization’s strategy to eliminate cervical cancer.
A Nationwide HPV Vaccination Drive Focused on Prevention
The government’s upcoming campaign will target girls aged 14 years, an age identified by global health bodies as offering maximum preventive benefit. The vaccine will be provided free of cost and administered at designated government facilities, including Ayushman Arogya Mandirs (Primary Health Centres).
Importantly, this will be a special vaccination drive, not part of India’s Universal Immunisation Programme. Vaccination under the national campaign will remain voluntary, ensuring informed consent while guaranteeing equitable access across socio-economic groups.
All vaccination sites will be linked to 24/7 government health facilities to ensure immediate medical support in case of adverse reactions, reinforcing both safety and parental confidence.
With this initiative, India will join over 160 countries that have already incorporated HPV vaccination into their national immunisation schedules. More than 90 countries worldwide have now adopted a single-dose HPV vaccination schedule, following updated global recommendations.
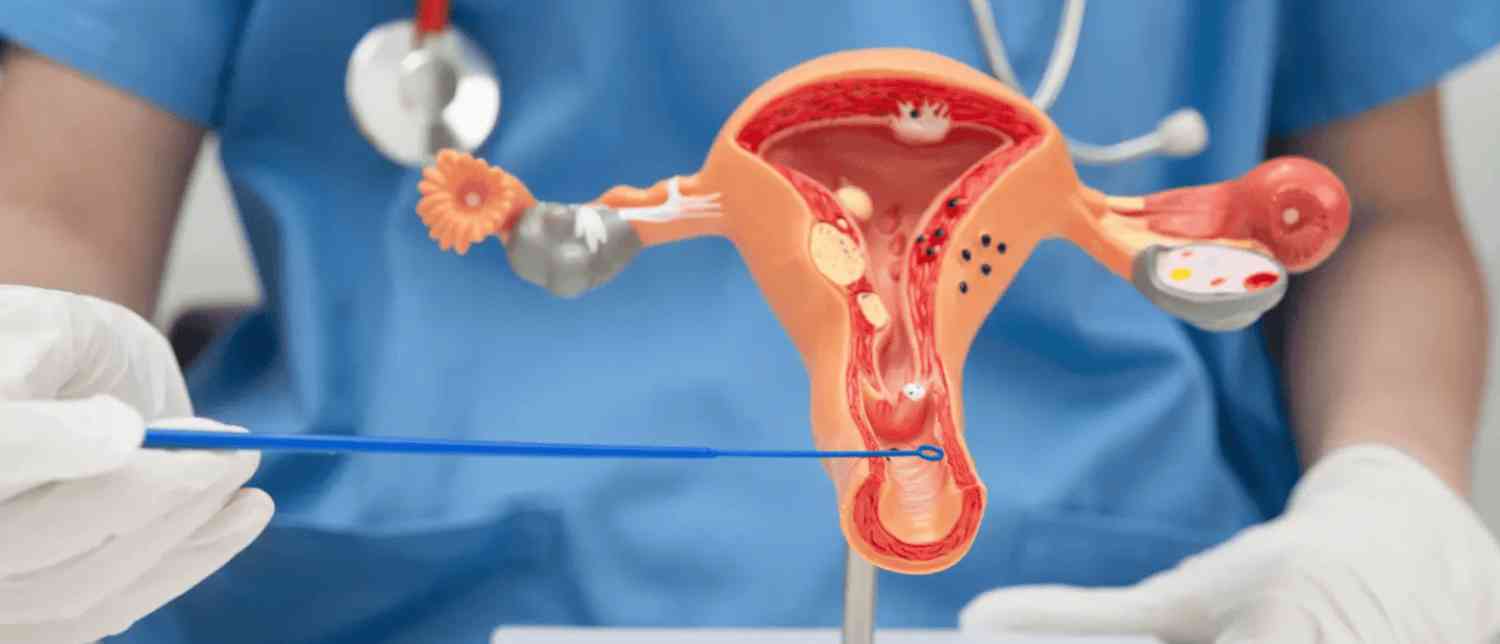
Why Cervical Cancer Demands Urgent Action in India
Cervical cancer remains the second most common cancer among women in India. Each year, the country reports nearly 80,000 new cases and over 42,000 deaths due to the disease. These numbers represent not just statistics, but thousands of preventable tragedies.
Scientific evidence confirms that almost all cases of cervical cancer are caused by persistent infection with high-risk types of Human Papillomavirus (HPV). In India, HPV types 16 and 18 alone account for more than 80 per cent—approximately 83 per cent—of cervical cancer cases.
Persistent infection with these high-risk strains gradually transforms healthy cervical cells into cancerous ones. By intervening before infection occurs, vaccination offers a powerful tool to drastically reduce this burden.
An official source cited by PTI emphasised that strong global and Indian scientific evidence confirms that a single dose provides robust and durable protection when administered to girls in the recommended age group. By prioritising prevention at the right age, the programme aims to deliver lifelong protection and significantly reduce future cancer incidence in the country.
What Is HPV? Understanding the Virus Behind Cervical Cancer
Human Papillomavirus (HPV) is a small, non-enveloped DNA virus. Unlike viruses surrounded by a fatty membrane, HPV is protected by a tough protein shell called a capsid. This capsid is composed of 72 star-shaped units that safeguard the viral genetic material.
There are more than 200 different genotypes of HPV, classified based on variations in their DNA sequence. The virus is epitheliotropic, meaning it specifically targets epithelial cells—the cells lining the skin and mucous membranes.
HPV typically enters the body through microscopic abrasions or tiny tears in the skin. Once inside, it travels to the basement membrane—the deepest layer of skin cells—where it hijacks basal cells and reprogrammes them to replicate viral DNA instead of performing their normal biological functions.
HPV types are broadly divided into low-risk and high-risk categories. Low-risk strains may cause common warts and are generally harmless. High-risk strains, particularly HPV 16 and 18, are far more dangerous.
These high-risk strains produce proteins known as E6 and E7. According to research from Johns Hopkins Medicine, these proteins disable the body’s natural tumour-suppressor proteins. When these protective mechanisms are shut down, cells begin to grow uncontrollably—laying the foundation for cancer development.
HPV spreads primarily through skin-to-skin sexual contact. While most infections are cleared naturally by the immune system, persistent infection over several years can trigger cellular changes that evolve into cervical cancer.
How Gardasil-4 Works: The Science Behind the Shot
At the centre of India’s vaccination drive is Gardasil-4, a quadrivalent HPV vaccine manufactured by MSD India, a subsidiary of Merck & Co. A quadrivalent vaccine is designed to protect against four strains of a virus. Gardasil-4 targets HPV types 16 and 18, responsible for cervical cancer, as well as types 6 and 11, which cause genital warts.
Crucially, the vaccine does not contain the live virus and cannot cause infection. Instead, it uses Virus-Like Particles (VLPs). These engineered proteins mimic the outer shell of the virus but contain no genetic material.
When injected, the immune system identifies these VLPs as foreign and mounts a defensive response, producing antibodies. These antibodies act like internal security guards, storing a blueprint of the viral structure.
If the vaccinated individual later encounters the real virus, the immune system recognises it immediately and neutralises it before it can infect cells.
A study published in The Lancet found that vaccination can reduce cervical cancer rates by almost 90 per cent when administered at a young age. Globally, HPV vaccines have demonstrated 93 to 100 per cent effectiveness in preventing cervical cancer caused by vaccine-covered HPV types.
Why the Government Chose Age 14
Some may question why the vaccination drive focuses on 14-year-old girls when puberty can begin earlier, sometimes as young as 8 or 9 years.
Doctors describe 14 as a “sweet spot” for public health implementation. It ensures vaccination occurs well before potential exposure to the virus while taking advantage of the hyper-responsive immune system of early adolescence.
Research from the National Cancer Institute shows that younger immune systems produce more antibodies in response to the vaccine than older ones. This strong immune response is the reason why global health authorities, including the World Health Organization (WHO) and the Centers for Disease Control and Prevention (CDC), recommend vaccinating children before exposure to HPV.
The WHO now supports a single-dose schedule for this age group, recognising that it provides sufficient antibodies to offer long-term protection.
Cost and Accessibility: A Major Barrier Removed
In the private market, Gardasil-4 is expensive. For girls below 15 years, it is administered in two doses, each costing ₹3,927. For individuals above 15 years, three doses are required.
By offering a single dose free of cost through government facilities, the national programme removes a significant financial barrier. This ensures that girls from all socio-economic backgrounds have equal access to life-saving protection.
The vaccine has a strong global safety record, backed by more than 500 million doses administered worldwide since its introduction in 2006. Widespread vaccination has led to substantial reductions in HPV infection rates, precancerous lesions, and cervical cancer incidence in several countries.
Common side effects are generally mild and may include soreness at the injection site or a low-grade fever. Decades of data from the CDC and WHO confirm the vaccine’s excellent safety profile.
Beyond Girls: Can Boys Benefit Too?
While the current government campaign focuses on girls, HPV is not gender-specific. It can cause cancers of the throat, head, neck, and other regions in men.
According to the Mayo Clinic, vaccinating boys contributes to herd immunity. When fewer individuals carry the virus, overall community transmission drops, indirectly protecting those who are unvaccinated.
In India’s private market, vaccines such as Gardasil-9 are available for both males and females up to age 45, offering protection against nine HPV strains.
A Step Toward Eliminating Cervical Cancer
India’s vaccination drive also coincides with the introduction of the country’s indigenous HPV vaccine, Cervavac, alongside Gardasil-4 in the public health system. Together, these vaccines strengthen India’s capacity to reduce and potentially eliminate cervical cancer for future generations.
The upcoming nationwide rollout has been described by official sources as a significant milestone toward achieving the vision of “Swastha Nari”—a healthy woman. The programme is built on three pillars: prevention, protection, and equity.
By targeting girls at the right age, offering vaccination free of cost, ensuring safety infrastructure, and aligning with WHO recommendations, India is embracing a science-driven strategy to combat one of its most persistent women’s health challenges.
Cervical cancer is largely preventable. With sustained implementation, public awareness, and high vaccination coverage, the country now stands at the threshold of dramatically reducing a disease that has claimed tens of thousands of lives each year.
In the coming years, the true measure of this initiative will not just be vaccination numbers, but the silent decline of new cancer diagnoses—and the countless lives saved before the disease ever takes root.
With inputs from agencies
Image Source: Multiple agencies
© Copyright 2025. All Rights Reserved. Powered by Vygr Media.